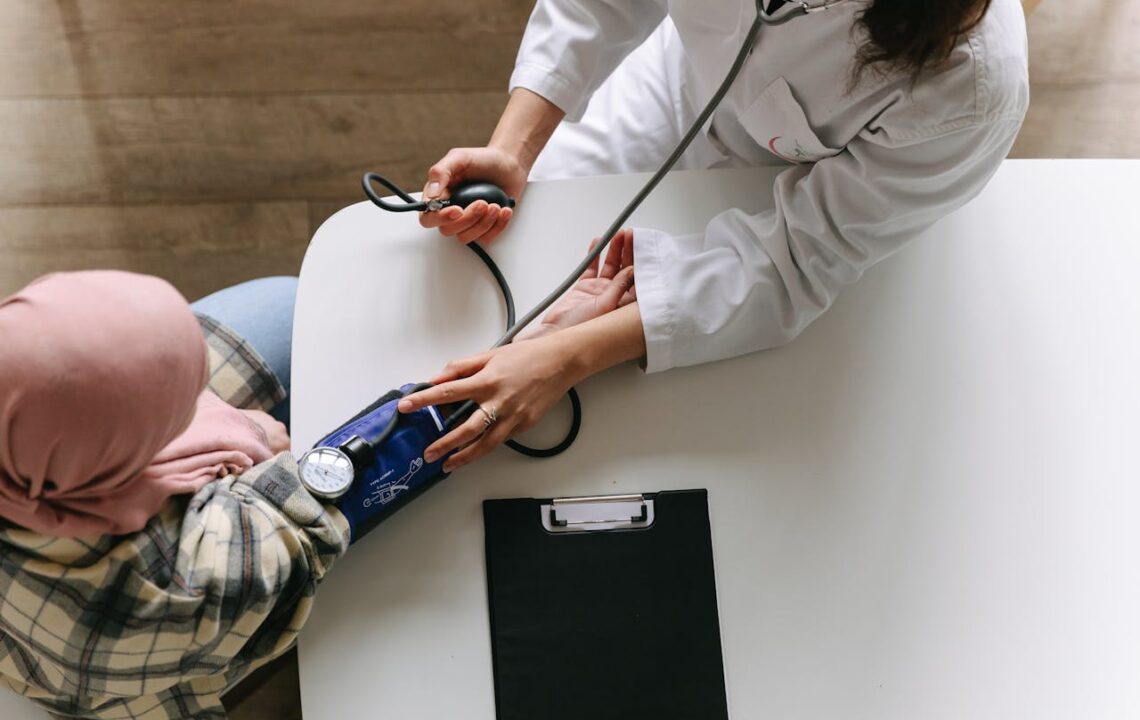
Every day, the heart pumps around 7,000 litres of blood through vessels spanning over 100,000 kilometres. The pressure at which blood flows through the arteries is one of the most important health indicators. And one of the most commonly overlooked. The difference between ‘normal’ and ‘optimal’ blood pressure may seem minor, but over the years it determines the risk of a heart attack, stroke, or kidney failure. Those two numbers on your blood pressure cuff deserve far more attention than most people give them.
Key facts about blood pressure:
- 120/80 mmHg marks the line between normal and optimal blood pressure and that gap matters more than most people realise
- Even a modest rise increases the risk of stroke and heart disease
- Hypertension builds silently over years without a single symptom – earning its reputation as the silent killer
- Just 30 minutes of walking a day can lower systolic blood pressure by 5-8 mmHg
- Dietary potassium acts as a natural antihypertensive – bananas, spinach, and avocados are among the best sources
Why should you know your blood pressure?
Elevated blood pressure doesn’t hurt and produces no warning signs – it quietly damages the vessels for years before the body sends a single alarm signal. The upper value (systolic) reflects the force with which the heart pumps blood, while the lower value (diastolic) captures the pressure in the vessels as the heart rests between beats.
The result is recorded in millimetres of mercury (mmHg) and typically looks something like this: 120/80. Even small deviations from the norm strain the heart and blood vessels with every beat – 24 hours a day, 365 days a year. That’s why knowing your numbers matters long before the body sends any warning signs.
Elevated readings damage the arteries and raise the risk of a heart attack and stroke. On the other hand, unusually low readings can trigger dizziness, fainting, and poor oxygen supply to the organs. The body regulates blood pressure continuously. Through the nervous system, hormones, and kidney function, but these mechanisms lose precision with age.
What are healthy blood pressure readings?
Healthy falls below 130/85 mmHg, but truly optimal readings – those that best protect the heart and vessels – sit below 120/80 mmHg. A meta-analysis published in The Lancet found that every additional 10 mmHg above the optimal level raises the risk of stroke by 20%. It’s worth aiming not just for readings that are ‘within range’, but for values that support long-term cardiovascular health.
Blood pressure categories according to cardiology guidelines:
- Optimal – below 120/80 mmHg, the lowest risk of cardiovascular disease
- Normal – 120-129/80-84 mmHg, acceptable values with a healthy lifestyle
- High normal – 130-139/85-89 mmHg, requires monitoring and lifestyle changes
- Hypertension – 140/90 mmHg and above, qualifies for treatment
What is the difference between optimal and normal blood pressure?
Optimal (below 120/80 mmHg) means the arteries are working under ideal conditions – without excessive strain or micro-damage. Normal (120-129/80-84 mmHg) still falls within a safe range, but the blood vessels are already exposed to slightly greater mechanical stress with every heartbeat.
The difference becomes apparent over the long term. A person with optimal pressure over 20 years will subject their vessels to far less cumulative strain than someone whose readings sit at the upper end of normal. Mechanical stress causes the arteries to stiffen gradually, which in turn drives even higher – creating a vicious cycle that’s far easier to prevent than to break.
Why does blood pressure rise with age?
The arteries lose elasticity with each passing decade. Collagen in the vessel walls gradually replaces elastin, making the arteries stiffer and less able to absorb the pressure wave generated by the heart. After the age of 50, systolic rises in almost everyone – even those who lead an active lifestyle.
This process is accelerated by excessive salt intake, a lack of physical activity, obesity, and chronic stress. With age, the kidneys become less efficient at regulating blood volume and sodium levels. The sympathetic nervous system becomes overactive, keeping the vessels in a state of constriction. That’s why regular checks after the age of 40 can detect changes long before any symptoms appear.
How to lower blood pressure without medication?
Lifestyle changes can lower blood pressure just as effectively as a single antihypertensive drug. Regular physical activity – even 30 minutes of brisk walking a day – reduces systolic pressure by 5-8 mmHg. Cardio exercises improve vessel elasticity, strengthen the heart, and lower the resting heart rate.
The DASH diet (Dietary Approaches to Stop Hypertension) is one of the most thoroughly researched eating plans for people with elevated blood pressure. It’s based on vegetables, fruit, whole grains, and a sodium limit of 2,300 mg per day. Combining the DASH diet with regular exercise delivers results comparable to pharmaceutical treatment.
Effective ways to lower blood pressure:
- Cutting salt intake – no more than one teaspoon a day (5 g)
- Increasing potassium intake from bananas, avocados, and spinach
- Reducing body weight – every kilogram lost by roughly 1 mmHg
- Limiting alcohol to one glass per day
- At least 150 minutes of physical activity per week
- Adequate sleep – 7-8 hours every night
Which foods help lower blood pressure?
Beetroot, garlic, olive oil, and oily fish are among the foods with the strongest evidence for lowering blood pressure. Potassium plays a central role because it acts as a natural sodium antagonist. Helping the kidneys flush out excess salt and relaxing the walls of blood vessels. A potassium-rich diet can lower systolic by as much as 4-5 mmHg without changing any other aspect of the diet.
Foods that support healthy blood pressure:
- Beetroot – contains nitrates that widen blood vessels
- Garlic – naturally lowers and improves blood flow
- Olive oil – protects vessels against inflammation
- Dark chocolate (at least 70% cocoa) – flavonoids support arterial elasticity
- Oily fish – omega-3 fatty acids lower blood pressure and protect the heart
Blood pressure and stress – the hidden link
Chronic stress is one of the most common yet underestimated drivers of elevated blood pressure. When the body enters fight-or-flight mode, the adrenal glands release adrenaline and cortisol. The heart beats faster, the vessels constrict, and blood pressure spikes. In the short term, this is a perfectly normal defence response.
The problem arises when stress persists for weeks and months. Elevated cortisol keeps blood pressure at a consistently high level. The kidneys retain more sodium and water, placing additional strain on the cardiovascular system. People exposed to chronic workplace stress have a 22% higher risk of developing hypertension.
Stress reduction methods that benefit blood pressure:
- Deep diaphragmatic breathing – lowers blood pressure within minutes
- Mindfulness meditation – regular practice reduces blood pressure by 4-5 mmHg
- Walks in nature – 20 minutes in a forest lowers cortisol by 16%
- Cutting caffeine during peak-stress hours
- A consistent sleep schedule supports vascular recovery
How to measure blood pressure correctly at home?
A single reading at the doctor’s surgery tells you surprisingly little about your true blood pressure – the ‘white coat’ effect inflates results in as many as 30% of patients. Regular home monitoring eliminates this bias and reveals the real picture. Modern health monitoring technologies make it easier to track results and spot concerning trends.
Rules for accurate blood pressure measurement:
- Measure morning and evening, before eating and taking any medication
- Sit comfortably with your back supported and feet flat on the floor
- Don’t talk or move during the measurement
- Place the cuff at heart level on a bare upper arm
- Take 2-3 readings 1-2 minutes apart and record the average
Simple habits for healthy blood pressure
Swapping salt for herbs, taking the stairs, adding a handful of nuts to your meals. Even these small changes can bring blood pressure down. There’s no need for a drastic overhaul – a few mindful choices repeated daily are enough. Monitor your pressure regularly and notice how it responds to your new routine. Even a modest drop – just 5 mmHg – translates into a significantly lower risk of stroke and heart attack over the years.
FAQ: Frequently asked questions about blood pressure
What blood pressure reading is dangerous?
A reading above 180/120 mmHg constitutes a hypertensive crisis requiring immediate medical attention, while values consistently exceeding 140/90 mmHg indicate hypertension that needs diagnosis and treatment.
Does coffee raise blood pressure?
Caffeine temporarily raises blood pressure by 5-10 mmHg for roughly 30-60 minutes, but in regular coffee drinkers the body develops a tolerance and the effect is considerably weaker.
How quickly can you lower blood pressure?
Breathing and relaxation techniques can lower blood pressure within minutes, whereas a lasting reduction through lifestyle changes typically requires 4-12 weeks of consistent effort.
Is low blood pressure dangerous?
A reading below 90/60 mmHg can cause dizziness, fainting, and reduced oxygen supply to the organs, but in many people – particularly younger and physically active individuals – it’s simply a normal variant that doesn’t require treatment.
References:
- Whelton, P. K., et al. (2018). 2017 ACC/AHA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults. Journal of the American College of Cardiology. https://doi.org/10.1016/j.jacc.2017.11.006
- Ettehad, D., et al. (2016). Blood pressure lowering for prevention of cardiovascular disease and death. The Lancet. https://doi.org/10.1016/S0140-6736(15)01225-8
- Sacks, F. M., et al. (2001). Effects on Blood Pressure of Reduced Dietary Sodium and the Dietary Approaches to Stop Hypertension (DASH) Diet. New England Journal of Medicine. https://doi.org/10.1056/NEJM200101043440101