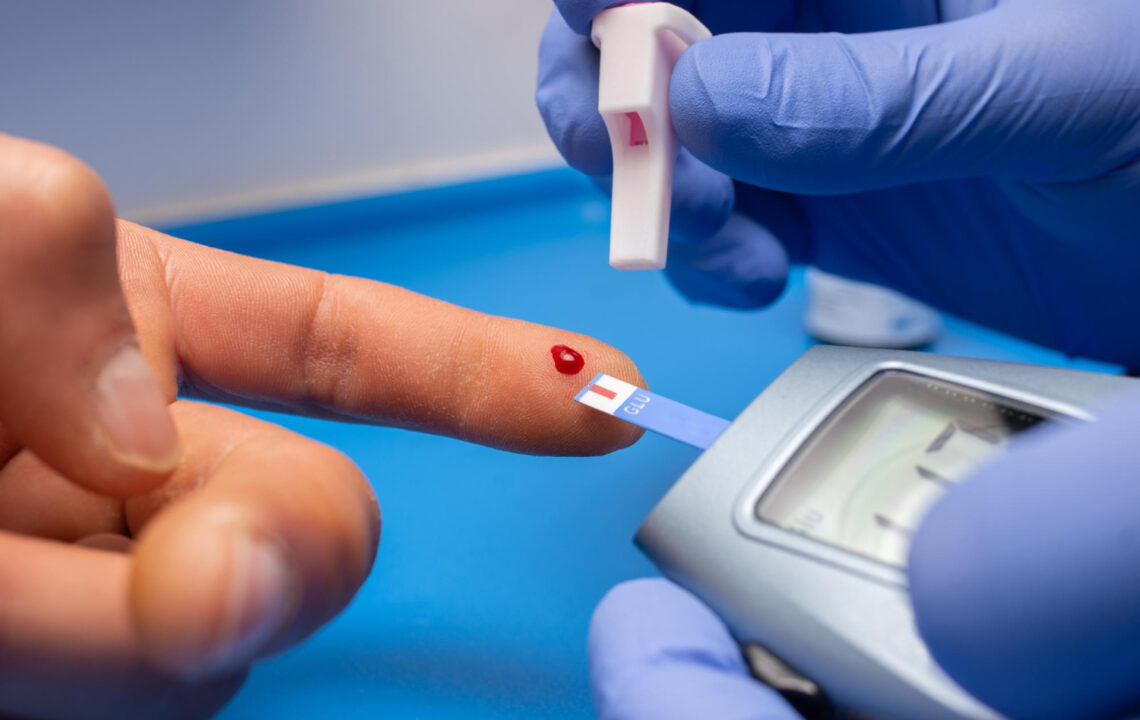
After years of daily blood sugar checks and taking tablets, your doctor says: you can stop the medication. For a growing number of people with type 2 diabetes, this is a reality backed by clinical trials. Lifestyle changes can reverse the condition – even after years of pharmacological treatment. Discover what truly affects blood sugar levels and how scientists define diabetes remission.
What you should know about type 2 diabetes:
- Remission is achievable in people who change their diet and lose weight within the first years of diagnosis
- Glycated haemoglobin (HbA1c) below 6.5% without medication is the criterion for remission
- Losing 10-15 kg restores normal insulin secretion in most patients
- 30 minutes of moderate exercise daily significantly improves insulin sensitivity
- A low-glycaemic diet cuts post-meal glucose spikes by up to 40%
Can type 2 diabetes really be cured?
For decades, type 2 diabetes was considered irreversible – a diagnosis meant medication for life. Last few years have changed that view. The DiRECT trial led by Professor Roy Taylor at Newcastle University found that 46% of participants achieved remission after one year of intensive dietary intervention. Key factor was losing at least 10 kg.
Cure and remission, however, are different concepts. Medicine avoids the word “cure” when it comes to diabetes because the condition can return. Remission means the body manages glucose regulation without medication – but it requires maintaining new habits. Those who reverted to their old diet lost the gains within a matter of months.
What helped DiRECT trial participants:
- A low-calorie diet (800-900 kcal daily) for the first 3-5 months under medical supervision
- Gradual reintroduction of normal food with an emphasis on vegetables and protein
- Regular weight monitoring – maintaining the loss was key to lasting remission
- Dietitian support and check-ups every 2-4 weeks
How does diabetes remission differ from a cure?
Reversal of the condition means maintaining HbA1c below 6.5% for at least three months without taking diabetes medication. This definition was adopted by the American Diabetes Association in 2021. A cure would imply permanent removal of the cause, yet type 2 diabetes involves metabolic changes that can reactivate. That is why clinicians speak of remission – a controlled state that still demands vigilance.
Type 2 diabetes – what do the latest studies tell us?
The latest epidemiological data show that type 2 diabetes accounts for roughly 11% of global deaths – making it one of the conditions that shorten life expectancy the most. On average, a diagnosis at age 50 means losing 6-8 years of life compared with healthy individuals. These figures, however, improve markedly for patients who take active preventive steps.
The UK Prospective Diabetes Study, spanning over 20 years, demonstrated that intensive glucose control reduced the risk of microvascular complications – damage to small blood vessels – by 25%. Blood pressure control proved equally important – a reduction of 10 mmHg cut stroke risk by 44%. This confirms that the link between diabetes and lifestyle rests on solid clinical evidence.
How does lifestyle affect type 2 diabetes?
Modifiable factors dominate the causes of type 2 diabetes – excess weight, physical inactivity, a diet rich in processed foods, and chronic stress. Genes create a predisposition, but lifestyle determines whether the disease develops. A large-scale prevention programme showed that changing habits reduced the risk of developing diabetes by 58%, whilst diabetes medication (used exclusively under a doctor’s direction) achieved only 31%.
Modifiable risk factors for diabetes:
- Excess visceral fat – fat around internal organs disrupts insulin signalling
- A sedentary lifestyle – fewer than 150 minutes of weekly exercise doubles the risk
- A highly processed diet – too much simple sugar and trans fats damage the pancreas
- Chronic stress – cortisol raises blood glucose and worsens insulin sensitivity
- Sleep deprivation – fewer than 6 hours of sleep increases insulin resistance by 40%
Intermittent fasting is one method gaining increasing scientific support for improving insulin sensitivity. Restricting the eating window to 8-10 hours a day gives the pancreas a rest and lowers fasting glucose. It is important to introduce this approach gradually and under medical supervision – particularly for those taking blood-sugar-lowering medication.
How to lower blood sugar naturally
The cornerstone of non-pharmacological glucose reduction is a low-glycaemic diet – built around foods that raise blood sugar slowly. Vegetables, legumes, wholegrain products, and healthy fats form a menu that stabilises glycaemia throughout the day. Glycaemic index and glycaemic load are tools that help make informed food choices.
Simple ways to lower glucose without medication:
- Meal sequencing – vegetables and protein first, carbohydrates last (reduces the glucose spike by 30-40%)
- Post-meal walks – 15-20 minutes of walking supports glucose uptake by the muscles
- Apple cider vinegar – a tablespoon before eating slows carbohydrate digestion
- Soluble fibre – porridge, beans, and apples form a gel that slows sugar absorption
- 7-8 hours of sleep – sleep deprivation raises cortisol and worsens insulin sensitivity
Insulin resistance – how many kilograms do you need to lose?
Losing 5-7% of body weight improves insulin sensitivity in most people with insulin resistance. For someone weighing 90 kg, that is just 4.5-6.3 kg. It sounds modest, yet the metabolic payoff is large – fasting blood sugar drops, glycated haemoglobin falls, and the lipid profile, meaning cholesterol and triglycerides, improves. With a 10-15% reduction, the chances of fully reversing the condition reach 60-70% (in patients diagnosed within the past six years, based on a controlled clinical trial).
What role does physical activity play in type 2 diabetes?
The link between physical activity and diabetes is one of the best-documented relationships in preventive medicine. Skeletal muscles take up glucose from the blood independently of insulin during exercise – which is why movement lowers blood sugar immediately. Regular training also increases the number of insulin receptors on cell surfaces, permanently improving tissue sensitivity to insulin.
The most effective forms of activity:
- Brisk walking – 30 minutes daily lowers HbA1c by 0.5-0.7 percentage points
- Resistance training – builds muscle mass, the body’s largest glucose “store”
- Cycling – engages large muscle groups whilst sparing the joints
- Swimming – ideal for those carrying excess weight, as it relieves the musculoskeletal system
How many minutes of daily exercise reduce insulin resistance?
The World Health Organisation recommends at least 150 minutes of moderate activity per week – roughly 22 minutes a day. Research shows, however, that even a 10-minute post-meal walk significantly lowers post-prandial glycaemia. Those who exercise for 300 minutes weekly achieve nearly twice the improvement in insulin sensitivity. Every additional minute of movement counts.
When is reversing diabetes more difficult?
The chances of remission diminish with disease duration – beyond 6 years, the probability of full reversal drops below 30%. Beta cells, which produce insulin, gradually become exhausted, and after 10-15 years secretory function may decline by 50-80%. Before changing your diet or lifestyle, consult your doctor – even partial improvements in habits lower the risk of complications.
FAQ: Frequently asked questions about type 2 diabetes
Does lifestyle affect type 2 diabetes?
Lifestyle changes – including diet, physical activity, and weight loss – reduce the risk of developing diabetes by 58% and enable remission in nearly half of patients with a short disease history.
Does this work after 60?
People over 60 derive comparable benefits from lifestyle modifications, though the pace of weight loss may be slower – the DPP study showed a 71% risk reduction in this age group.
What are the chances for someone with diabetes for fewer than 4 years?
Patients diagnosed up to 4 years earlier have the highest chance of remission – in the DiRECT trial, 60% of those with a short disease duration achieved HbA1c below 6.5% without medication after one year of intervention.
Which low-glycaemic diet works best for remission?
A diet based on vegetables, legumes, wholegrain products, and healthy fats, with limited simple sugars and highly processed foods, delivers the best results in lowering glycated haemoglobin.
References:
- Lean, M. E. J. et al. (2018). Primary care-led weight management for remission of type 2 diabetes (DiRECT): an open-label, cluster-randomised trial. The Lancet. https://doi.org/10.1016/S0140-6736(17)33102-1
- UK Prospective Diabetes Study Group (1998). Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes. The Lancet. https://doi.org/10.1016/S0140-6736(98)07019-6
- Knowler, W. C. et al. (2002). Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. The New England Journal of Medicine. https://doi.org/10.1056/NEJMoa012512